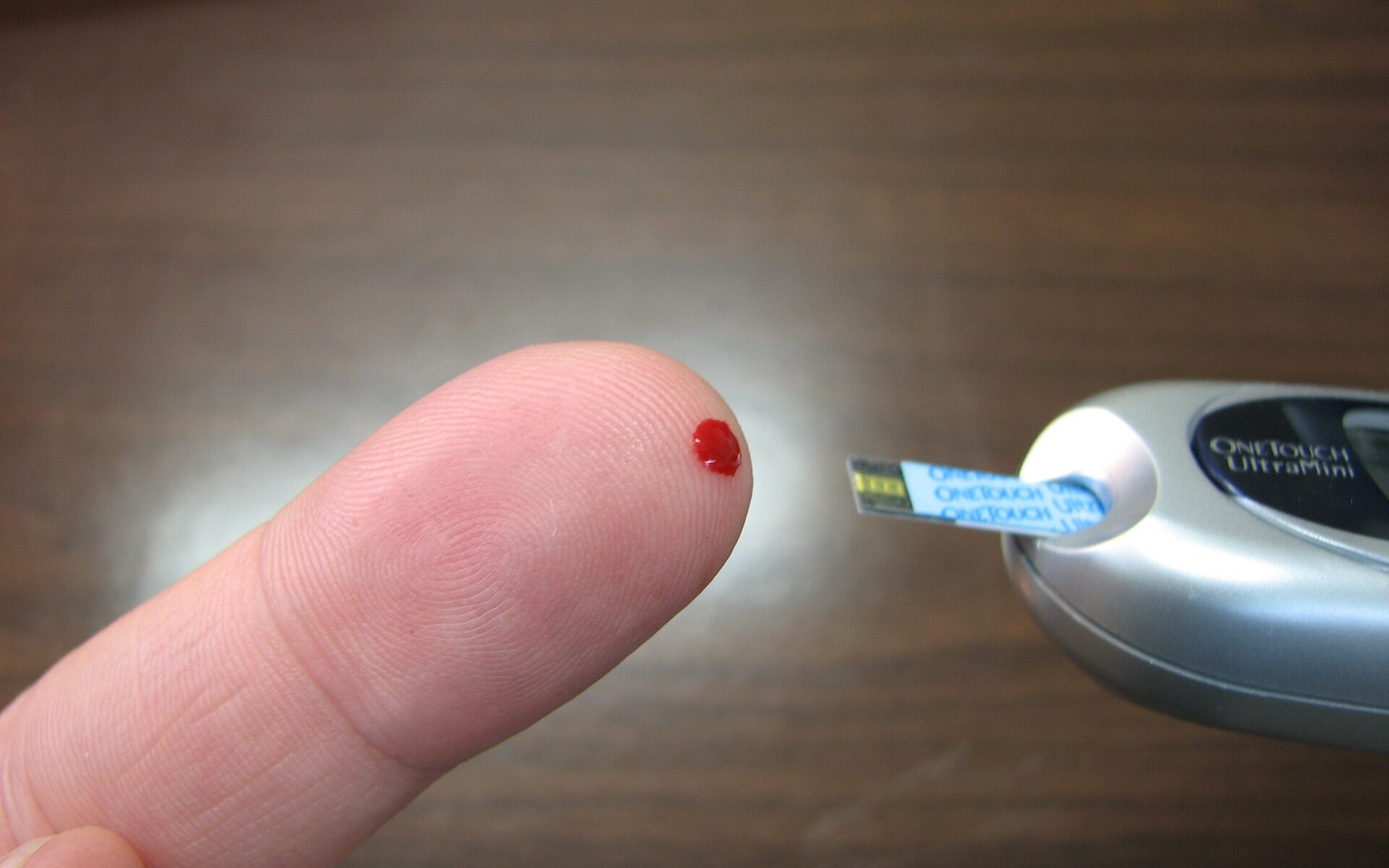
Diabetics test their blood sugar several times a day. They do this to check that medications are working as they should, and to see if their blood sugar is too high or too low.[1]
If blood sugar levels are too far outside the norm for a diabetic, that can be a serious health risk.
Why would someone diagnosed with prediabetes choose to self-monitor? It’s not a standard recommendation, but maybe it should be.
If you’ve been diagnosed as prediabetic, you probably get your A1C[2] tested every few months or annually to see if you’ve developed type 2 diabetes. You go to the lab, get a blood draw, and you’re done.
Kind of important to know if you’ve moved from prediabetes to type 2 diabetes.
But, the A1C test is not the only test that is used to diagnose diabetes.
After all, according to the experts, you only need two days of fasting plasma glucose at or greater than 126 mg/dL to be diagnosed diabetic.[3]
It’s possible to be prediabetic and develop full-blown diabetes between those occasional A1C tests.
Self-monitoring your blood sugar can alert you to full-blown diabetes, or that you’re dangerously close to it. This awareness gives you time to immediately stop what you’re doing and try to correct course.
It also helps you to learn what your body tolerates in the way of food and drink, and it shows you what exercise does to your blood sugar levels.
Self-monitoring allows you to learn at a granular level just what’s happening with your blood sugar, and what you can do to affect it.
Use a blood sugar monitor (also called a meter) to discover exactly where your blood sugar is – if you’re prediabetic, normal, or officially a type 2 diabetic.
If you believe you have developed full-blown diabetes, you’ll want to have that confirmed by your healthcare provider, and a medical plan will be put into place.
“Eat to your meter” is a phrase you may hear when chatting to other prediabetics. It means you use the meter to guide you away from foods that make your blood sugar levels go up. Or conversely, toward foods that sustain you and don’t throw your blood sugar out of whack.
Since the goal is to get your blood sugar to stay down in the normal range, rather than the prediabetic range (and definitely not in the diabetic range), it’s necessary to eat more of this and less of that. What “this” and “that” is depends on your body, and that’s what eating to a meter can help you figure out.
Some prediabetics can eat carbs from, say, a carrot or even a carrot cake, and their blood sugar blips up then back down. Other prediabetics will get a big long-lasting bounce in their blood sugar if they eat carbs from the same sources.
Because prediabetes can cause some of the same problems as full-blown diabetes, it’s time to get aggressive in the fight against elevated blood sugar.
According to a thoroughly unscientific interview process performed through an online support group, prediabetics who choose to use a meter seem to find that they use it a lot early on. After a few months, they don’t use it as much because they’ve learned what works for them and what doesn’t.
Changes in lifestyle (food choices, exercise levels, weight control) based on what the meter is saying help them move toward normal levels of blood sugar, and soon they find they don’t need to use a meter to know what they should be eating and how much they should be exercising.
If you decide to start using a meter, you can buy one over the counter in your local pharmacy.
Be aware that insurance doesn’t always cover the cost of the meter and the strips.
Each meter will be slightly different so read the instructions before use, but these are the basic steps to using a meter:
- Wash and dry your hands and then, if possible, use an alcohol wipe on the pad and sides of a fingertip. This is for infection control and to remove any substance which might affect the test results.
- Insert a strip into the meter.
- Use the included needle to poke the pad or side of your fingertip. No need to aggressively stab yourself. Keep it shallow, just enough to draw a tiny bit of blood. Squeeze around the hole to get a drop of blood if it isn’t immediately evident.
- Touch the strip as indicated to the drop of blood, and your meter should tell you your blood sugar level after a few seconds.
Talk with your healthcare provider about what numbers you should be looking for, but generally speaking, as prediabetics our goal is to have numbers in the normal (rather than prediabetic) range:
- before a meal the meter should read between 70 and 99 mg/dl (3.9–5.5 mmol/L) for normal blood sugar levels
- two hours after a meal the meter should read less than 140 mg/dl (7.8 mmol/L) for normal blood sugar levels
It’ll be helpful to note what you’re eating. This makes it easier for you to remember foods and amounts that work for you.
Using apps such as the popular Carb Manager (free) or Carb Manager Premium (not free) is a common way to do this. (We are not associated with Carb Manager, but we do use the app.)
There are dozens of helpful apps, so choose one that makes the process of tracking foods and whatever else you want to track the easiest for you.
If you check your blood sugar before eating and it is 105 (a little higher than normal because you’re prediabetic) and two hours after you start eating a banana it is 145, then next time, try eating half a banana. Or cut bananas from your list of foods. For now.
Remember, the goal is to identify how individual foods affect your blood sugar levels, and to stay away from those that make it stay elevated.
[1] Mayo Clinic, Blood sugar testing: Why, when and how, https://www.mayoclinic.org/diseases-conditions/diabetes/in-depth/blood-sugar/art-20046628, (May 20, 2019).
[2] National Institute of Diabetes and Digestive and Kidney Diseases, Diabetes Tests & Diagnosis, https://www.niddk.nih.gov/health-information/diabetes/overview/tests-diagnosis, (May 20, 2019).
[3] https://www.niddk.nih.gov/health-information/diabetes/overview/tests-diagnosis.